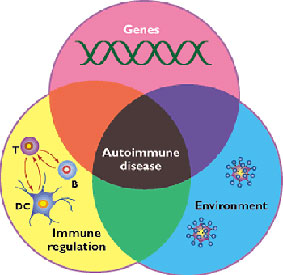
 Vitiligo carries a strong association with other autoimmune conditions, such as type 1 diabetes, pernicious anemia, Addison’s disease, systemic lupus erythematosus, rheumatoid arthritis, and polyglandular autoimmune disease. Histological evidence further supports an autoimmune etiology.
Vitiligo carries a strong association with other autoimmune conditions, such as type 1 diabetes, pernicious anemia, Addison’s disease, systemic lupus erythematosus, rheumatoid arthritis, and polyglandular autoimmune disease. Histological evidence further supports an autoimmune etiology.
Vitiligo lesions have an infiltrate of inflammatory cells, particularly cytotoxic and helper T cells and macrophages. This infiltrate is most prominent in the perilesional skin just prior to the clinical appearance of vitiligo.
Additional studies have shown that patients with vitiligo often have elevated levels of antibodies against melanocyte antigens such as tyrosinase and tyrosinase-related proteins 1 and 2.
Population case-control analyses have also shown associations between vitiligo and human leukocyte antigen (HLA) alleles. Significant examples include HLA-DR4, which is associated with antibody-mediated autoimmune diseases such as type I diabetes mellitus and cicatricial pemphigoid, and HLA-Cw6, which is also associated with psoriasis.
By investigating families with vitiligo and other autoimmune diseases, researchers at the University of Colorado have found that certain chromosomal locations are associated with inheritance among these relatives. Of these, the locus 17pl3 was determined to contribute to vitiligo and systemic lupus erythematosus. Recently, they discovered that certain polymorphisms of a gene within this region, the NALP1 gene, are associated with an increased risk of generalized vitiligo and vitiligo-associated autoimmune disease.
This was initially described in a study of 114 Caucasian families in the US and UK and was later confirmed in a population-based case control study of unrelated Romanian patients with generalized vitiligo. The product of this gene, NALP1, is an important part of the innate immune system and is highly expressed in T cells and Langerhans cells.
As Langerhans cells are especially active in the epidermis, this may be evidence of an autoimmune reaction occurring specifically in the skin. The NALPl protein has pyrin domains and in its natural form detects bacterial motifs for innate immune defense. Pyrin gene mutations also play a role in Muckle-Wells syndrome (urticaria, deafness, and amyloidosis), familial Mediterranean fever, and the PAPA (pyogenic sterile arthritis, pyoderma gangrenosum, and acne) syndrome.
Another recent genetic study identified a polymorphism in the melanocortin-1 receptor (MC1R) gene that is associated with protection against vitiligo. This gene encodes the melanocyte stimulating hormone receptor (MSHR) which, when bound by [alpha]-MSH, stimulates eumelanin production through a cAMP response.
Single nucleotide polymorphisms (SNPs) of the MC1R gene have already been associated with red hair and/or fair skin and a susceptibility to skin cancer. In studying 108 vitiligo patients and 70 controls from a fair-skinned Hungarian population, Szell et al found that the C478T SNP in the MC1R gene was significantly higher in the control group. This SNP leads to an Arg l60Trp amino acid change in the second intracellular loop of the MSHR protein, a component of the protein kinase C target sequence.
This location suggests that the SNP may confer protection against vitiligo by altering signal transduction events. However, the authors note that computer-assisted prediction shows that the mutation also creates an epitope with a lower antigenicity. Therefore, they propose that this SNP may function by providing protection against an autoimmune process.

