 Vitiligo is an autoimmune pigmentation disorder that destroys the melanocytes (cells which make pigment) leaving skin and hair depigmented. Melanocytes in vitiligo patients, whether in normal or depigmented skin, are inherently different from those in people without vitiligo. This “difference” may make them uniquely vulnerable. What triggers and drives their destruction?
Vitiligo is an autoimmune pigmentation disorder that destroys the melanocytes (cells which make pigment) leaving skin and hair depigmented. Melanocytes in vitiligo patients, whether in normal or depigmented skin, are inherently different from those in people without vitiligo. This “difference” may make them uniquely vulnerable. What triggers and drives their destruction?
Researchers around the world are investigating the complex interplay of genetics, environmental events, biochemical and immunological events that are believed to be involved in this process of destruction. The process is generally believed to be driven by an autoimmune dysfunction causing the immune system to produce antibodies or cytotoxic T cells, that normally kill virally-infected cells and tumor cells, but instead destroy the body’s own melanocytes. Several other autoimmune disorders occur at increased frequencies with vitiligo, such as autoimmune thyroid disease, Addison’s disease, pernicious anemia, rheumatoid arthritis, psoriasis, type 1 diabetes, and systemic lupus erythematosus, confirming the autoimmune connection discovered by the genetic research of Dr. Richard Spritz and his team at the University of Colorado. Their research has linked several genes found in vitiligo patients to this “family” of autoimmune diseases.
There are several theories as to what is triggering and influencing this autoimmune dysfunction. Many believe that this likely means that vitiligo is the result of a multi-faceted set of factors, including a complex set of genes, stress, accumulation of toxic compounds, infection, autoimmunity mutations, and impaired melanocytes. Research is focused on understanding this interplay of factors in order to improve existing therapies and, for the first time, be able to design therapies to stop depigmentation.
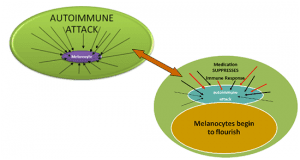
Current vitiligo therapies such as topical steroids, topical immunomodulators (non-steroidal alternatives that affect the function of the immune system without the side effects associated with topical steroids), excimer laser, narrowband UVB (NB-UVB), and psoralen plus UVA (PUVA), are aimed at suppressing the immune response so that the melanocytes once again flourish and repigment the skin.
These therapies are used according to the type and severity of the vitiligo. For example, topical and laser therapies would typically be used primarily to treat smaller, isolated lesions of vitiligo, whereas full body NB-UVB or PUVA would be used to treat more widespread vitiligo. Though these conventional therapies were initially developed for other skin diseases, they are also moderately effective in vitiligo. By suppressing the immune system’s dysfunction and stimulating melanocyte growth, these treatments can help the skin regain its pigment.
In recent years, various topicals, such as topical immunomodulators (tacrolimus or pimecrolimus), have been successfully combined with NB-UVB to shorten treatment time and speed up repigmentation. Other combinations are now being tested, as well as adaptations of other conventional drugs.
In addition to improving our ability to suppress the immune response through adaptations of existing therapies, we may eventually have the capacity to interrupt the immune response that results in vitiligo. Several researchers are looking at ways to interrupt the biochemical signaling that leads to the depigmentation of the skin. The object is to prevent depigmentation by interrupting the cascade of biological events leading to the destruction of melanocytes. The progression of existing vitiligo would be stopped and depigmented skin would be able to naturally repigment. Normal messaging would be restored, thereby enabling the body to once again produce the healthy melanocytes needed for pigmentation. If successful, this research could lead to more effective and safer methods of control, and constitute the first therapies uniquely designed to treat or prevent vitiligo.


